Validating Sterile Filtration: Overcome the Fear of Failure
For a process as critical and sensitive as sterile filtration, it’s not surprising that many filter end-users experience some “fear of failure.” As risk management consultant Peter Sandman has said, people become fearful when they feel they are not in control [1]. As a result, some may see established sterile filtration practices as inadequate. Compelled by fear to do more than necessary, they may overdesign their filtration systems, adding wasteful and costly procedures.
By embracing this fear, rather than studying the root causes of filter penetration and the specifics of each process, practitioners of sterile filtration impede the advancement of filtration science and its understanding within the industry and global regulatory agencies.
This article will examine several unnecessary practices that are burdened upon the industry today, using process validation principles to explain why they are inadequate. It will also touch on problems that result when “model organisms” used to evaluate sterile filters are seen as universal archetypes that can characterize all process situations and filter types.
First, let’s consider the concept of validation itself, which is designed to “establish documented evidence which provides a high degree of assurance that a specific process will consistently produce a product meeting its pre-determined specifications and quality attributes [2].
Validation is a global regulatory requirement for drug manufacturing, particularly for aseptic processes. As industry consultant Jim Agalloco has written [3], there is already a substantial body of knowledge on best validation practices for sterile injectable biotech products, including:
Fluid influences on the organisms, membrane polymer and retention mechanism
Process parameter influences on the membrane polymer, filter construction and retention mechanism
Validated processes are under control, yet their reliability continues to be questioned by regulators and those in the field, suggesting that many practitioners do not fully understand the validation concepts. This can often be traced to subjective fears rather than valid technical concerns.
Here are some examples of current concerns, requirements or practices, pulled directly from regulatory or company documents, that illustrate that fear:
“0.2-µm filters can be penetrated by microorganisms, so the industry must switch to 0.1-µm-rated filters.”
• “Increasingly, there are detectable but non-culturable organisms or L-forms or nano-bacteria in our processes.”
• “Redundant 0.2-µm filtration is necessary and should be used.”
• “I need an absolute 0.1- or 0.2-µm filter.”
• “Diffusive flow integrity testing is better than bubble point testing.” (Currently, there is a difference in preference between U.S. and European regulators)
• “Flawed filters will not be detected by a post-use test, as the pore will be plugged during filtration.”
• “The maximum bioburden in front of a sterilizing filter should be 10cfu/100mL.”
We will address many of these statements individually, later in this article.
The question is: does the most widely used model organism always reflect specific process and filter characteristics?
Beyond Size Exclusion: There Is No Universal Model Organism
Brevundimonas diminuta is typically used as the model for organisms that are expected to be found in pharmaceutical manufacturing environments. It was selected, based on its presence in pharmaceutical operations, and within native bioburden [4].
The organism has been found particularly suitable for validating sterilizing grade filters due to its size and ease of cultivation. However, it should only be used to model situations where its dimensions closely match the organisms of interest in a given application, relative to the filter pore size and shape.
Furthermore, in some cases, sieve retention may not be the mode of organism removal. For instance, in some cases, it may be adsorption, as the organism forms hydrogen bonds to the filter’s polymeric surface. This could account for the observation, 26 years ago, that Pseudomonas aeruginosa organisms are more strongly retained by polyamide membranes than by cellulose triacetate filters [5]. It also explains the removal of latex particles from aqueous suspensions by polyamide membranes in the presence of surfactant, but not in its absence (Table 1) [6].
Table 1: Retention (%) of 0.198-µm spheres by various 0.2-µm-rated membranes
| Filter Type | In Water (% ) | In 0.05% Triton X-100 (%) |
| Polycarbonate | 100.0 | 100.0 |
| Asymmetric polysulfone | 100.0 | 100.0 |
| Polyvinylidene fluoride | 74.8 | 19.2 |
| Nylon 66 | 82.1 | 1.0 |
| Cellulose esters | 89.4 | 25.1 |
From Tolliver and Schroeder (1983) courtesy of Microcontamination
B. diminuta should not be viewed as a universal model organism, as some native bioburden may be a better alternative as challenge organism, being close to the actual process settings. Unfortunately, rare penetrations of sterilizing grade filters have caused an exaggerated doubt in the reliability of filtration. Appropriate process validation though should render such doubts and be trusted by even the most critical reviewer of sterile filtration..
Sources of Variability: Size and Shape
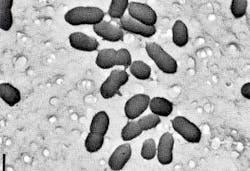
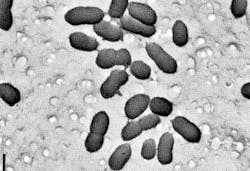
B. diminuta varies in size and shape, depending on how it is cultivated. Back in 1967, Bowman and colleagues described the B. diminuta size as 0.3 × 1.0 μm [7]. However, in 1978, Leahy and Sullivan found [8] that the organism grown at 30 °C and incubated for 24 hours in saline lactose broth, a minimally nutritional medium for that microbe, yielded cocci-like cells approximately 0.3 × 1.0 μm (Figure 1). Similar considerations have to be accounted for when challenge tests are performed with native bioburden forms.
B. diminuta are typically cultivated to develop as spherical a form as possible, since spheres are least amenable to retention. Thus, Leahy and Sullivan proposed, back in 1978, that it be used as the model organism for 0.2/0.22-μm-rated membranes, partly because of its size relative to the 0.2-μm dimension [8].
Subsequently, the FDA designated it for that very purpose [9], defining a sterilizing filter as one that retains a minimum of 1 x 107 cfu of Brevundimonas diminuta ATCC 19146 / per cm2 of effective filtration area (EFA).
Although it isn’t the smallest organism known, B. diminuta was considered diminutive enough to represent whatever smaller organisms were likely to be present in pharmaceutical preparations. The smaller the test organism, goes the logic, the more likely that its removal by a filter would assure the sieve retention of larger organisms.
However, ease and safety of cultivation and handling are also important considerations. In 2001, Sundaram and colleagues found an increasing number of cases where filtration in 0.2/0.22-µm-rated membranes failed to yield sterile effluent [10]. Experimental studies showed that penetrating organisms had shrunken because they had been cultivated in broths that were nutritionally inadequate. In such cases, the physicochemistry of the suspending fluid may serve to alter the size of the suspended organisms as expressed by the Donnan equilibrium consequent to ionic strengths.Organism Shrinkage During Processing
Sundaram’s team [11] also found that organisms underwent size changes after exposure to certain drugs. In cases with 0.2-µm-rated membranes, the researchers found, the larger pore size could only provide sterile effluent and/or a high titer reduction with regard to certain organisms for various lengths of time, before penetration occurred.
Penetration times varied from 24 to 96 hours, and the cumulative challenge at which penetration was first observed ranged from 1.2 x 107 to 1.1 x 108 cfu/cm2. Two 0.2-µm rated Nylon-66 filters in series were unable to fully retain Ralstonia pickettii (now Burkholderia pickettii) with penetration observed at 72 hours, corresponding to a cumulative challenge of 2.4 x 107 cfu/cm2. The more extensive penetration of the Nylon-66 membranes, compared with the PVDFs, is in keeping with their greater degree of openness, as Krygier and colleagues showed in 1986 [12].
As a result, it has been suggested that 0.1-µm-rated membranes be substituted for their 0.2-µm-rated counterparts.
Sundaram’s team evaluated five 0.1-µm-rated membranes and found that they yielded sterile effluent over the entire duration of the test (120-196 hours), up to challenge levels of 5.7 x 107 to 2.0 x 108 cfu/cm2. Similar results were obtained with the PVDF filters tested; no B. pickettii were detected at challenge levels of 5.9 x 107-6.0 x 108 cfu/cm2.
In addition, all 0.1-µm-rated filters tested provided consistent and complete retention of B. pickettii for the entire duration of the test (120-192 hours), suggesting that the smaller pores would ensure sterile product at conditions where penetration could occur through conventional 0.2- and 0.22-µm-rated sterilizing grade filters. Proponents argue that using 0.1-μm-rated membranes would permit longer term formulation and filtration operations. In fact, 0.1 µm-rated filters may be the best choice for long-term filtrations.
However, penetration has also been found in 0.1 µm-rated filters. In 1999, Sundaram’s team found that B. pickettii, when its size was so affected, could be retained by certain 0.1-µm-rated filters. But, in a similar situation, they found that only four of seven commercially available 0.1-μm-rated membranes could remove a particular organism. Just because one type of membrane so classified may provide proper retention, does not mean that any other 0.1-µm-rated membrane can also be depended upon for a like result.
It is important to remember that today, there are no industry standards by which 0.1 filters can be judged. In addition, more research clearly needs to be done into the kinetics behind the organism’s size changes, evaluating different organisms in different fluids.
Based on available data, long term filtrations may best be handled by 0.1-µm-rated filters, subject to validations being performed. However, in other cases, substituting 0.1-µm-rated for 0.2-µm-rated membranes may be unnecessary, and could result in significant penalties, including:
Slower flow and processing rates, resulting in longer term operations.
Higher costs for larger EFAs
More leaching and extractables
Higher product losses, due to adsorptive bonding to the ultimately greater filter area used.
A responsible choice requires that both the 0.1 µm-rated membranes and the 0.2 µm-rated membranes be validated.
If both types of filter prove appropriate, the higher pore size rating should be used to avoid the penalties of reduced flows. If, however, the validation data do not permit a clear resolution, the 0.1 µm-rated membranes should be used, since retention is more critical than flow rate or flux.
Below, we address some of the common sterile filtration concerns, requirements or practices that appear to be motivated by fear and can best be resolved by careful process validation.
“0.2-µm filters are penetrated by organisms. The industry is, therefore, required to switch to 0.1-µm-rated filters.”
In certain specific processes, 0.2-µm–rated filter can be penetrated by organisms, or by organisms which would normally be retained by such filters. In such cases, the flltrative removal of the organisms may well require the use of 0.1 µm–rated filters. Such instances are not new. Their occurrences have been considered by regulators for years, at least since the PDA and FDA held a special forum on this topic in 1995 [13].
Certain organisms, such as Burkholderia pickettii, Burkholderia cepacia, and Pseudomonas aerugenosa. shrink as a result of their immersion in fluid media that are only minimally nutritious for them [14]. Their reduction in size renders as invalid validations that use B. diminuta as a model. Brevundimonas diminuta can undergo shape alterations in minimally nutritious media but is not listed as undergoing size alterations occasioned by contacts with process fluids.
The fact that some microbes require 0.1-µm–rated filters to arrest them does not signify that all organisms are so disposed. The necessitated switch from 0.2-µm-rated to 0.1-µm–rated happens in only roughly 0.005% – 0.01 % of sterilizing grade filtration applications.
A mandated switch is therefore scientifically and statistically unfounded. Its promulgation may be shunned and process validation activities and data used as performance verification. Sole reliance on pore size ratings have been found obsolete anyway.
“Increasingly there are detectable but non-culturable organisms or L-forms or nano-bacteria in our processes.”
Conclusions cannot be made regarding the sterile filtration of microorganisms unless the methods of quantifying them by culturing and counting are available. Organisms such as the L-forms, nanobacteria, and “viable but non-culturable” entities may not be amenable to such analyses. Concerns about their presence may be justified, but without the means to cultivate and count them, it is impossible to attest to their complete absence.
It follows that a sterilizing filter can be judged only by its performance in the removal of identifiable and culturable organisms known to be present in the drug preparation [15]. The complex of influences governing the outcome of an intended sterilizing filtration necessitates a careful validation of the process, including that of the filter [4]. The very drug preparation of interest, the exact membrane type, the precise filtration conditions, and the specific organism type(s) of concern must be employed in the necessary validation.
“Redundant 0.2-µm filtration is necessary and should be used.”
Not necessarily. Again, proper process validation will disclose whether a single filter will do the job or not. However, there are some specific applications which traditionally, for whatever reason, utilize a second (redundant) filter as an “insurance filter,” i.e. if the first filter fails, the second may compensate. This holds, however, only when each filter has been validated to show specified retentivity.
Even so, the wisdom of the exercise deserves careful evaluation, as it assumes added costs for membrane EFA, increased leachables and extractables. The loss of drug product may needlessly be incurred by the filter’s heightened product hold-up, and unspecified adsorption.
“The maximum bioburden in front of a sterilizing filter should be 10 cfu per 100 mL of fluid.”
This is true if one wishes to accord with EMA regulations, and especially if one wishes to export product to Europe. The FDA makes no such stipulation, but bases its approval on process validation.
Seemingly in conflict, the two views arise from the same premise. The EMA regulation tries to establish the same sterility assurance level (SAL) for filtration as for thermal sterilization. EMA recognizes that, the greater the number of challenges, the more likely that at least one will succeed.
The FDA seems to agree, in that if the filter can sustain the removal of organism burdens far above those liable to be encountered in real life situations, it can assuredly withstand lesser insults. If, as the authors see it, the FDA’s massive challenge fails to breach the filter’s pores, it is needless to compel bioburden assessment in front of the filter. Filter validation would gainfully serve the intended purpose. Process validation, effectively conducted, would reliably demonstrate the filter action.
“I need an absolute 0.1- or 0.2-µm-rated filter.”
As a former FDA authority, since retired, once observed, “The word ‘absolute’ should be used only in conjunction with vodka.” Absoluteness implies a complete independence from conditions, an inherent ability to retain particles larger that than the filter’s pore size rating, regardless of any other considerations. Without a complete knowledge of the properties of the particles and filter pores at our disposal, the statement is devoid of technical significance or guidance. It may, perhaps, be used in ignorance (although cynics may suspect that its utility derives from marketing efforts, a practice not unknown in the competitive world of sales.)
Control vs. Fear
As Sandman elucidated, human beings like to be in control, and, if this status cannot be achieved, may move rapidly to fear. Unfortunately, when sterile filtration is concerned, fear can result in the installation of wasteful, unnecessary safety nets that can create more problems than they solve.
Being in control is the desired state, and such control can only come from process validation studies. Their authority is at least as old as Lord Kelvin’s basic scientific principle, “When you can measure what you are speaking about, and can express it in numbers, you know something about it.”
It speaks to validation. In sterile filtration, as in most areas of pharmaceutical manufacturing, science-based validation is the best cure for fear.
References
1. Hessler, A., Sandman, P.M. Squeaky Clean? Not Even Close. http://www.nytimes.com/2004/01/28/dining/squeaky-clean-not-even-close.html?sec=health?pagewanted=1
2. FDA. Guideline on General Principles of Process Validation, FDA CDER, 1987.
3. Agalloco, J.P. “Compliance Risk Management Using a Top-Down Validation Approach,” Pharmaceutical Technology, July 2008.
4. PDA Technical Report 26 (2008), Sterilizing Filtration of Liquids, Parenteral Drug Association, Bethesda, MD.
5. Ridgway, H.F., Rigby, M.G., and Argo, D.G. “Adhesion of a Mycobacterium to Cellulose Diacetate Membranes Used in Reverse Osmosis.” Applied and Environmental Microbiology 47, 1984, pp. 61-67.
6. Tolliver, D.L. and Schroeder, H.G. “Particle Control in Semiconductor Process Streams.” Microcontamination (l), 1983, pp. 34-43 and 78.
7. Bowman, F.W, Calhoun, M.P. and White, M. “Microbiological Methods for Quality Control of Membrane Filters.” J. Pharm. Sci., 56/2, 1967, pp. 453-459.
8. Leahy, T.J., Sullivan, M.J. “Validation of Bacterial Retention Capabilities of Membrane Filters.” Pharmaceutical Technology 2(11), 1978, pp. 64-75.
9. FDA. Guideline on Sterile Drug Products Produced by Aseptic Processing, FDA CDER, 1987.
10. Sundaram, S., Eisenhuth, J., Howard Jr., G.H., and Brandwein, H. “Part 1: Bacterial Challenge Tests on 0.2 and 0.22 Micron Rated Filters.” PDA Journal of Pharmaceutical Science and Technology, 55 (2), 1984, pp. 65-86.
11. Sundaram, S., Auriemma, M., Howard Jr., G.H., Brandwein, H., and Leo, F. “An Application of Membrane Filtration for Removal of Diminutive Bioburden Organisms in Pharmaceutical Products and Processes,” PDA Jour. Pharm. Sci. and Technol. 53 (4), 1999, pp. 186-201.
12. Krygier, V. Rating of Fine Membrane Filters Used in the Semiconductor Industry, Transcripts of Fifth Annual Semiconductor Pure Water Conference, (1986), pp. 232-251, San Francisco, CA
13. PDA/FDA Special Scientific Forum, Bethesda, MD; Validation of Microbial Retention of Sterilizing Filters, July 12-13, 1995.
14. Mittleman, M.W., Jornitz, M.W., Meltzer, T.H., “Bacterial Cell Size and Surface Charge Characteristics Relevant to Filter Validation Studies,” PDA Jour. of Pharm. Sci. and Technol. 52 (1), 1998, pp. 37-42.
15. Agalloco, J., Letter to the Editor—re: “It just doesn’t matter, It just doesn’t matter, It just doesn’t matter.” PDA Journal of Science and Technology. Vol 52, No. 3, pp. 149-150.