Mission Possible: Excellent Clinical Logistics
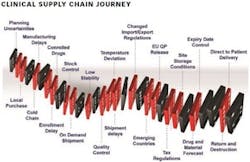
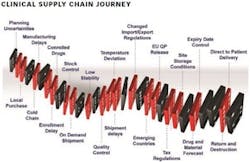
The clinical trial supply chain is a conglomerate of many individual, sometimes multifarious, links that must be reasonably assembled to form a stable chain. It’s not simply a linear row consisting of a few simple tasks.
There are essential supply chain elements to consider when integrating third-party providers, especially with contract manufacturing organizations (CMOs), as well as best practices to improve information flow among clinical, logistics, manufacturing and IT teams.
QUALITY
Favorable clinical trials are those having a positive effect on the tested substance. Certainly, patient safety is a key focus. Formulation of the investigational product, its stability and all associated packaging aspects are essential in this regard. Sometimes good manufacturing practice (GMP) efforts to finish a product are underestimated by clinical R&D personnel. The only appropriate response for CMOs is to consistently educate sponsors and CRO stakeholders. Implementation of robust quality/technical agreements should be a given.
Recognizing the highest impact and importance of quality within the supply chain is a basic but often neglected element. Without an elaborated quality management mindset that embraces the supply chain, a clinical trial may not be successful. Quality does not start or finish with product manufacturing, however, it is one essential part that should never be omitted. The final study result is valuable only when all processes have been developed well in advance and when all possible known consequences have been thoroughly considered. The awareness of the field of work in which we are operating must be omnipresent and repeatedly verified.
BULLWHIP EFFECT
Who has not experienced the bullwhip effect in clinical supply chains? Due to limited transparency of demands along the supply chain — from the patient, investigator, clinical monitor, local depot, central distribution center, CMO or third party vendor involved in pre-production activities — last-minute orders or misuse of available stock hinders trial continuity and produces considerable inventory swings. This can not only have dramatic cost implications, but may also impact safety. Patients already enrolled into a clinical trial can be put at risk if not supplied with sufficient trial medication on time.
To make clinical logistics more efficient, one must understand the dependencies and evaluate and mitigate associated risks in advance. A single weak link in the chain can cause the entire ensemble to break.
Clinical supply planners are challenged with evaluating several aspects during the start-up phase, however, they often find themselves disconnected from the clinical team. Since CMOs are involved early in the supply chain stage of production, it is essential to embed manufacturing experts into the clinical trial core planning structure. CMOs must know the expected delivery time to sites and patients, as well as the required quantity and availability of the initial IMP batch. Likewise, they must have information about drug product shelf life and stability, which are essential for expiry management and drug handling at sites/patients.
[javascriptSnippet]
A forward-looking distribution strategy includes the entire manufacturing element as part of the overall plan, forming a coherent, logical process long before packaging is complete. Expiry date management and distribution schemes should also be factored into the strategy. Packaging and label design, plus the impact of product characteristics — dosage form, temperature conditions — must also be considered.
Biopharmaceutical R&D experts and CROs are wise to integrate CMOs into planning stages. They can get ahead even more if they implement a sales and operations planning (S&OP) model — the gold standard in the supply chain industry that fully loops CMOs and CROs into that process. This type of collaborative business process may help drastically reduce planning cycle time and improve forecast accuracy. It can also help mitigate the risk of stock-outs along the full supply chain. Additionally, processes also become more standardized and lean across all parties.
MANUFACTURING
Product formulation and stability, as well as IMP kit design — be it a study-specific labeled blister, bottle or vial — can significantly impact storage, distribution and administration. We have seen projects with relatively large blister packages shipped under cold chain requirements of 28°C. While this was obviously a lower cost for production, especially for relatively small batches of over-encapsulated drugs, they heavily affected transportation costs because air had to be transported in validated high-volume shippers. The same concept applies for the number of batches to be produced. At first glance it may seem less expensive to perform one larger production run than many smaller ones. However, by taking into account expiry dates, uncertain enrollment numbers and a high volatility in regional distribution demands, one large production can quickly become unusable while fresh batches are desperately needed.
CMOs can be more innovative by steadily optimizing manufacturing and implementing better processes, including: small-batch IMP labeling, forecast automation, production planning and resource allocation. Additionally, investments in future logistics areas, such as e-Labeling, RFID and On-demand/Just in Time labeling, can add value to clinical trials by supporting chain of custody.
Certain manufacturing process aspects can influence distribution, handling and re-supply processes. Although initial forecasts of product quantity are completed during the planning phase, the supply chain must be monitored closely to reduce potential disruption risks. The relentless review of planning parameters during the execution phase enables clinical logistics experts to adjust according to external factors that influence the flow. An elaborated plan at the outset helps simplify the drug development journey along the clinical supply chain, but in many ways the planning phase is a continuous activity.
TECHNOLOGY INTEGRATION
Combined with the elements outlined above, technology plays an important role in the journey. Over the years, clinical supply chain experts have instituted many technical instruments, including interactive response technology (IRT) solutions that streamline and simplify complex processes. These, in turn, enable more intelligent and cost-effective in-time supply distribution within the highly global and volatile clinical trial environment.
A key to success is tightly integrating enterprise technology — which combines manufacturing, storage, distribution, investigational site management and clinical trial management systems — with CMO distribution experts along the clinical supply chain. An enterprise resource planning (ERP) solution is considered the ultimate S&OP tool for the clinical trial logistics business. This fosters straighter technology integration, supports lean process management and creates reasonable calculation and more precise forecasts.
Manufacturing is an ambiguous process, which is why associated technologies and supply logistics must be flexible and provident. Frequent adjustments to initial assumptions must be included from the beginning and verified along the chain. If one link moves in an unexpected direction, it weakens the chain and requires modification. Minimal movements can adjust the flow so that the direction is realigned once again.
Efficient planning and proper technologies along the manufacturing chain can minimize overage, avoid product shortages and optimize production and packaging campaigns to support informed decision making. With the help of enterprise solutions, processes can be further streamlined and automated, improving operations and costs.
An effective and non-disruptive end-to-end clinical supply chain is possible if CROs, CMOs, logistics providers and the broader biopharmaceutical industry act together as trusted partners. One only needs to examine other business sectors such as the automotive or semiconductor industries to find benefits of collaboration. Having the CMO as a partner enables real communication and deeper cooperation that can lead to new and successful approaches to clinical trial logistics. Holistic project management, combined with an intelligent supply chain strategy, can generate successful outcomes at the end of the drug development journey.